When I was first diagnosed with a Mast Cell Activation Syndrome (MCAS), my GI doctor told me that when he got my biopsy results back, he expected to see a high eosinophil count also. And he was correct! That was before research had been completed on these two cellular disorders, and today it’s more common to hear mast cell patients talk about also having high eosinophil counts.
I haven’t heard of a lot of EoE patients, however, talk about high mast cell counts. Yet from my anecdotal evidence, I have spoken with many adults and families managing EoE who tell me about symptoms of their EoE that sounds VERY familiar with mast cell patients.
I believe there is big opportunity for more research on how these two cells interact, and how a patient who receives a diagnosis for one of these illnesses needs to be monitored for the other.
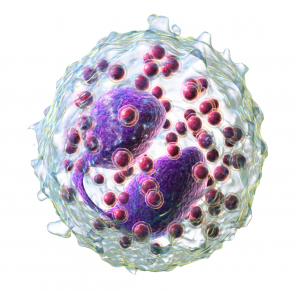
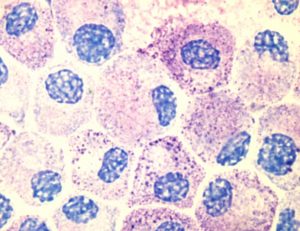
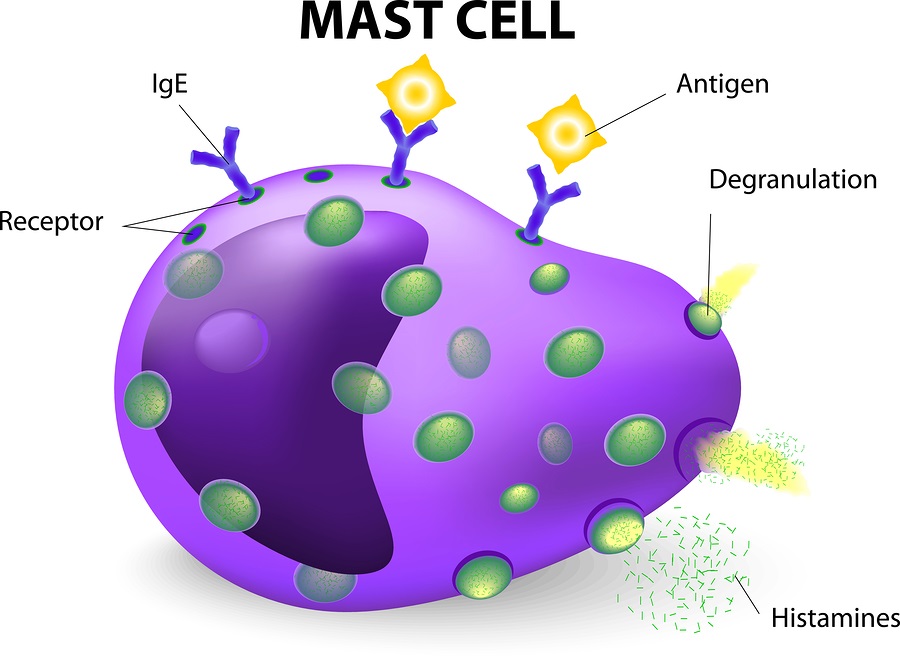
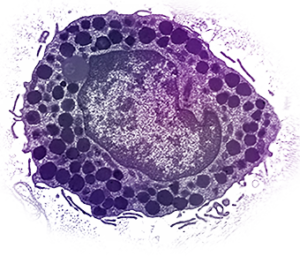
To my unscientific eye, these cells do look similar, however from the research we have now, we know that they don’t respond similarly to stimuli. In a 2014 research study, the authors found “Eosinophils were more viable when mast cells were present, dependent on soluble mediators and on physical cell contact…Mast cells were not as clearly affected or made more viable by eosinophil coculture.”
Further, the research found, “Both mast cells and eosinophils are present in biopsy specimens of patients with EoE. There is a great mast cell signature in EoE, and the presence of mast cells has been found to be useful in distinguishing between EoE and gastroesophageal reflux disease in biopsy specimens….IL-9 produced by mostly eosinophils served as a potent mast cell growth factor.”
Since I have a diagnosis of both MCAS and EoE, I can tell you that I have learned the difference of what the symptoms feel like for each of the illnesses. With EoE, I will experience the following symptoms in a flare (which is most likely to occur in the fall season): coughing, choking, gagging, acid reflux that I feel in my breast bone, and high stomach/lower esophagus pain, nausea and diarrhea. With MCAS, there isn’t as much of a season where I feel the symptoms. In general, I have some of these symptoms every day, to a greater or less degree: “hot flashes” with anxiety feelings after that, itchy skin and rashes, stomach pain, nausea and diarrhea. I have found that EoE affects the mucosal barrier of my gut much more than does MCAS. In other words, the eosinophil cells feel meaner and more destructive than the mast cells.
It’s difficult sometimes to know which illness is affecting me. I have found that for me certain medications work better to minimize the symptoms of one condition. Your own experience may be different! For me, Zyrtec helps MCAS but doesn’t do much at all for EoE. The mast cell stabilizer medication, Ketotifen, helps both MCAS and EoE, but is really effective for MCAS. The swallowed steroid, Asmanex, helps the EoE but doesn’t do much for the MCAS. Chinese herbs help both because the herbs aren’t geared toward one kind of cell, but instead work on inflammation in the body as a whole. That’s one of the reasons I like Traditional Chinese Medicine so much!
There are more drugs being researched that have been shown to decrease IL-5 (Interleukin 5) which is a cytokine involved in both MCAS and EoE. Mepolizumab, sold under the brand name Nucala, is one of these monoclonal antibody drugs, and has been studied for eosinophilic asthma and idiopathic mast cell activation and shows promise. We need more options to manage these two conditions, that although rare, can completely debilitate the patient and are becoming less and less rare.